What are cataracts
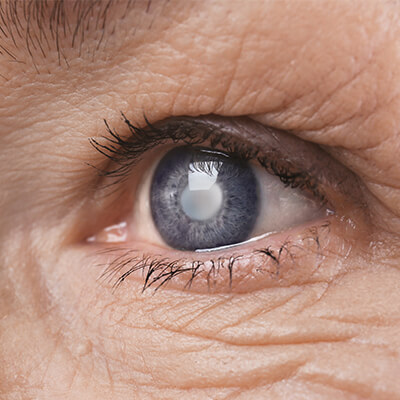
A cataract is formed when the natural lens of the eye, responsible for focussing light and producing sharp images, becomes cloudy and hardens, resulting in a loss of visual function.
A cataract is painless and usually develops gradually over several months or years. Normally, the onset of a cataract in one or both eyes may cause decreased night vision, impaired depth perception, and increased color distortion.
The cause of cataract formation is unknown, but scientists do know that a chemical change takes place within the lens of the eye with age. Cataracts are a part of the normal aging process, affecting 80 percent of people over age 60 (although not all cataracts are due to age). In fact, some babies can be born with cataracts, while some people develop them as a result of injury, prescription medication use or other causes.
Cataract Symptoms
- Blurred, fuzzy or hazy vision
- Feeling that there is a film over the eyes, or that one is looking through a veil or cobweb
- Frequent changes in eyeglass prescriptions
- Sever decrease of vision when looking at a bright scene or background
- Glare, halos or tails around headlights when driving at night
Though none of these symptoms necessarily mean you have a cataract, if you experience one or more, you should have your eyes examined by an optometrist or ophthalmologist.
Cataract Surgery
The only treatment for a cataract is surgical removal.
Years ago, when cataract surgery was less successful than today, cataracts were often not removed until the patient was almost blind. With advances in cataract surgery and intraocular lens (IOL) implants, it is no longer necessary for patients to wait until vision is severely impaired. Today, cataracts are usually removed at the point where visual impairment interferes with the daily activities of living – such as driving a car or reading.
Thanks to advances in microsurgical techniques, cataract surgery is performed without complications in more than 98 percent of cases.
The cataract removal is performed under a specially designed, high-powered microscope. The most common method of removal is called “phacoemulsification,” where a small incision is made near the outer edge of the cornea and the cataract is removed by dividing it surgically and then emulsifying it with ultrasound waves. The lens capsule is left in place to support the Intraocular Lens (IOL) implant. At a later time, the capsule behind the IOL implant may become clouded. This is known as a “secondary cataract” and may be treated by the use of a laser.
Intraocular Lens (IOL) Implantation
An intraocular lens (IOL) is used to replace the human lens during cataract surgery. This lens is typically made of acrylic, but it can also be silicone or polymethylmethacrylate (PMMA). It is usually implanted behind the iris, the colored portion of the eye, and cannot be seen. This is the natural position of the human intraocular lens.
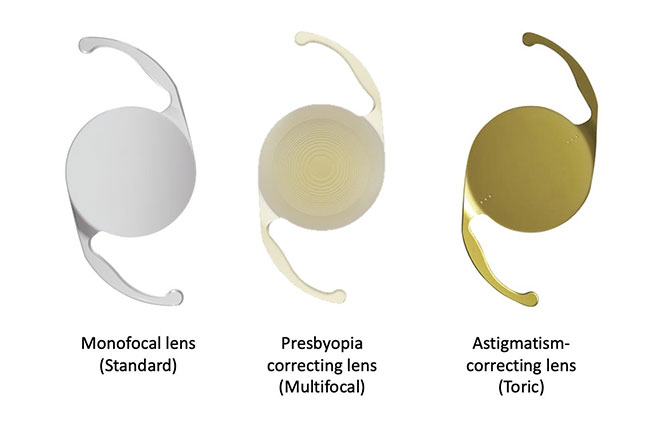
Different types of IOLs
The first IOL was implanted in 1949 by an English ophthalmologist, Harold Ridley. Since then, many advances in IOL design have occurred. Today, IOLs may be made from a plastic called polymethylmethacrylate (PMMA), silicon or an acrylic material, which has been found to be most compatible with the delicate tissue of the human eye. The latter two can be folded and inserted through a small sutureless incision.
How Long Does Cataract Surgery Take?
You will be in our facility at Glaucoma-Cataract Consultants for about two-three hours. You will be in the operating room for about twenty minutes, and the procedure itself will take about ten to fifteen minutes. After surgery, you will rest in comfort while you recover from the initial surgery before going home.
Will I Feel Any Discomfort During Cataract Surgery?
A nurse anesthetist will administer mild sedation to relax you and place eye drops to numb your eyes before the procedure.
Can I Wear my Contacts Until the Day of Cataract Surgery?
No, your contact lenses may change some of the measurements we take before the surgery. The staff at Glaucoma-Cataract Consultants will make sure you are given the proper instructions for the time period that we will need you out of your contact lenses.
Are There Any Restrictions After Cataract Surgery?
No, your contact lenses may change some of the measurements we take before the surgery. The staff at Glaucoma-Cataract Consultants will make sure you are given the proper instructions for the time period that we will need you out of your contact lenses.
Are There Any Restrictions After Cataract Surgery?
No heavy lifting more than 10 lbs or strenuous activity for 1 week after surgery. Do not rub your eye and do not get your eye wet for the first week after surgery. You should also avoid driving and alcoholic beverages for twenty-four hours. We advise you to postpone showering until after you see the doctor the next day.
Do Cataracts Ever Come Back?
No, cataracts don’t ever come back after surgery. However, there is a phenomenon called an “After cataract” which occurs in over 50% of people who have cataract surgery. This happens when scar tissue develops on the back of the implanted lens, causing cloudy vision. It can be easily treated in clinic with a laser procedure called a YAG capsulotomy.
